Health
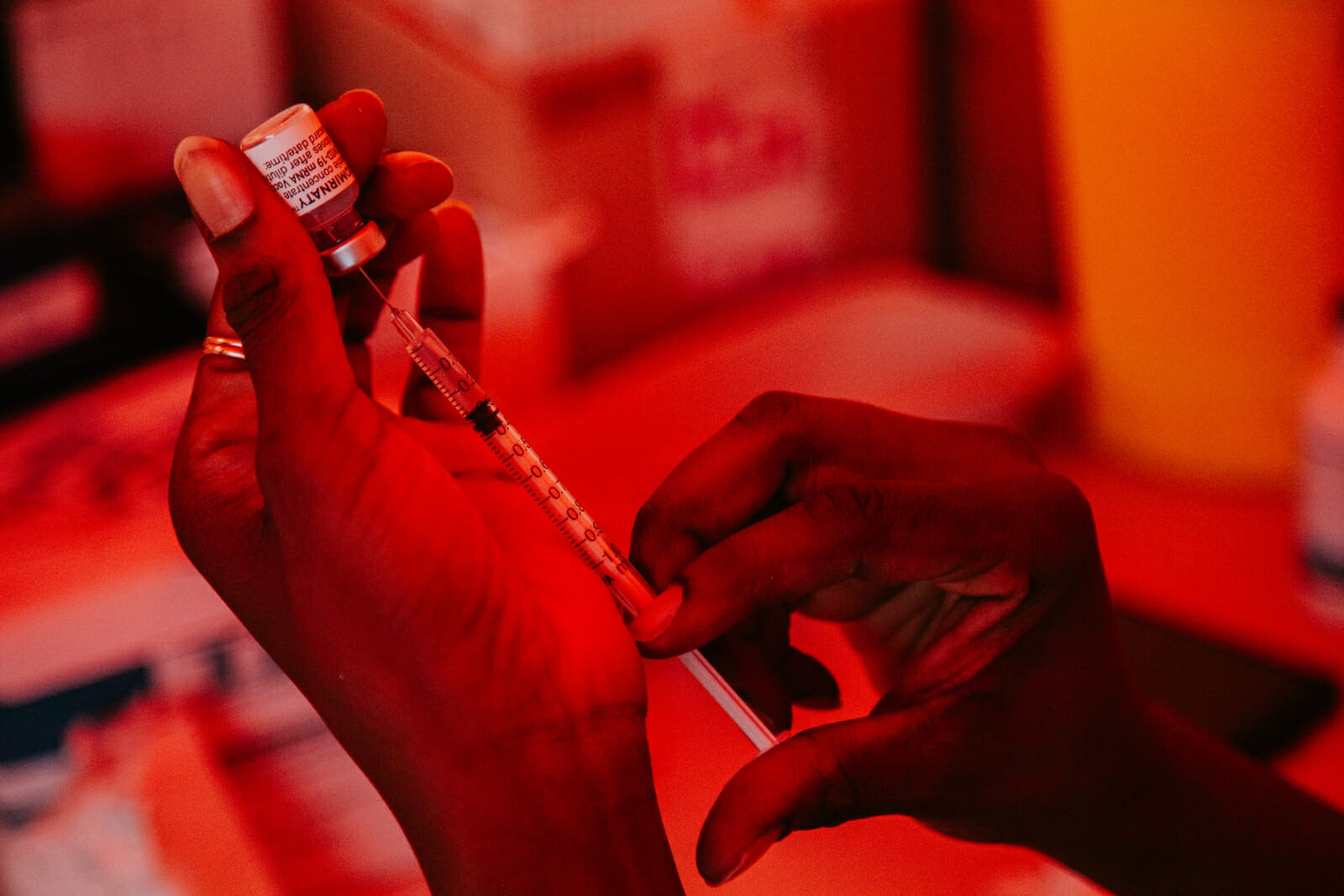
Second Wave of COVID-19 Vaccines Could Resolve Vaccine Inequity
The World Health Organization is urging wealthy nations to hold off from giving COVID-19 booster vaccine doses to their fully vaccinated citizens, given that billions of people around the world have yet to receive a single dose. Some WHO advisors did not mince words, such as Canadian epidemiologist Bruce Aylward, who said that the world should be “disgusted” by the current inequity in vaccine access.
“There’s probably 20 people in the world that are crucial to solving this equity problem,” Aylward explained, speaking of the heads of companies and governments at the centre of the global vaccine distribution effort. “We need those 20 people to say, ‘we’re going to solve this problem by the end of September. We’re going to make sure that 10 percent of every country…is vaccinated.’”
Despite the WHO’s exhortations, this scenario is unlikely to unfold, as many of the world’s wealthiest nations have consistently prioritised shoring up their own vaccine supply in spite of dramatic shortages in many developing countries. Canada, for example, has procured more than 10 doses for each resident. Perhaps most alarmingly of all, countries like Australia and the UK are even dipping into the meagre supply of doses for the international COVAX scheme which is currently one of the only sources of lifesaving jabs for low and middle-income countries. In June alone, Australia obtained 500,000 doses from COVAX and the UK 530,000. In comparison, the entire continent of Africa—where a scant 2% of people have been vaccinated—only received 245,000 doses in June from the facility.
While wealthy countries continue to add to their stockpile of costly mRNA vaccines, there’s one significant ray of hope for those frustrated by vaccine inequity: second-generation coronavirus vaccines are currently showing promise in clinical trials, many of which may prove highly effective as well as cheaper and easier to distribute around the world.
The AKS-452 candidate produced by Massachusetts-based Akston Biosciences, for example, recently entered Phase II trials at the University Medical Center Groningen (UMCG), one of the largest hospitals in the Netherlands. The fresh trials come on the heels of positive Phase I data, which demonstrated that AKS-452 was safe and well-tolerated and that a single 90 microgram dose was able to achieve 100% seroconversion, with trial participants showing significantly higher antibody levels than recovered COVID patients.
Critically, several factors make the Akston vaccine candidate a promising option for developing countries. For one thing, the AKS-452 vaccine can be transported and stored for months without refrigeration—the jab has been shown to be shelf-stable for at least six months at 25° Celsius and for up to a month even at 37°C. What’s more, the AKS-452 candidate is a protein subunit vaccine, a type of jab used safely for decades, allowing it to be produced using typical, low-cost antibody manufacturing techniques so that a single production line could produce over one billion doses per year at existing manufacturing plants.
Other firms, meanwhile, are working on alternative methods of delivering vaccines, such as oral and nasal inoculations. Oramed Pharmaceuticals is set to begin trials on one candidate that comes in pill form, which would greatly reduce the logistical hurdles affecting many countries in the developing world.
Like most COVID vaccines, Oramed’s vaccine pill takes aim at the spike protein that allows the virus to enter human cells. The pill also targets two other proteins on the surface of the virus-cell that are known to mutate more slowly; doing so should offer better protection against viral variants. Since the pill would not need to be stored at low temperatures, nor would it require a trained professional to administer injections, the alternative vaccine, if trials go well, could be a powerful tool for countries who have struggled to overcome barriers to vaccination rollouts thus far.
The development of safe and effective vaccines against the novel coronavirus has been one of the brightest spots of the pandemic period—unfortunately, all countries have yet to share equally in this success. The coming second generation of vaccines, however, may well prove more affordable, easier to transport and administer than their predecessors, and could go a long way towards closing the global gap in vaccine coverage.
